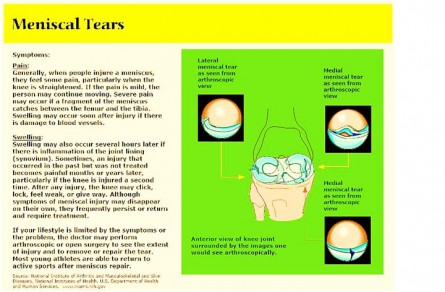
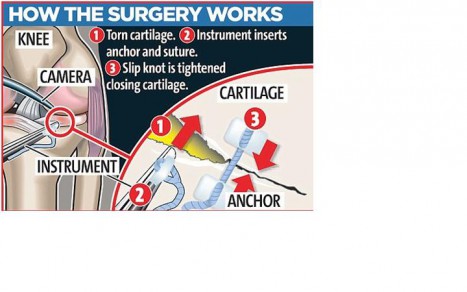
Figure 1. The doctor is in.
New research from Finland suggests that thousands of people who have arthroscopic knee surgery to fix a torn cartilage, might be wasting their time.
A report on the Finnish Degenerative Meniscal Lesion Study (FIDELITY), published recently in the New England Journal of Medicine, finds that the benefits of keyhole operations to repair degenerative meniscal tears are no better than sham operations.
Keyhole surgery or arthroscopy, is a procedure where the surgeon inserts a scope through a small incision to examine the joint and, if required, also partially removes the damaged cartilage through another incision.
Previous studies have shown that keyhole surgery on the knee does not help patients with osteoarthritis and such procedures have become less common for arthritis sufferers. In the meantime, keyhole surgery to repair torn cartilage has risen significantly, despite lack of evidence that it actually helps, says the Finnish team.
Knee problems other than arthritis that cause stiffness and pain are very common, and are caused most often by gradual wear and tear, rather than sudden injury or trauma. The most common diagnosis that requires treatment is a torn meniscus, a crescent-shaped cartilage that acts like a shock absorber and helps stabilize the knee.
Figure 2. Meniscal Tears.
Comparing partial removal of damaged cartilage with sham procedure.
In this new study, the Finnish team recruited 146 patients aged from 35 to 65 with meniscal tears that had developed through the wear and tear process as noted above. None of the patients had arthritis of the knee.
The researchers randomly assigned the patients to one of two groups: one underwent keyhole surgery to partially remove the damaged meniscus and the other underwent a sham procedure. In the sham procedure, the surgeons simulated the real operation. They manipulated the patient’s knee and handled surgical instruments near the knee so the patient was under the impression they were being operated on.
Consequently, both groups underwent arthroscopy, where the scope in inserted into the keyhole allowing the surgeon to look at the torn cartilage, but only one group actually had part of the cartilage removed. However, neither the patients, the people caring for them after the operation nor the researchers analyzing the results knew which patients had undergone the real procedure and which had just had the sham operation.
Both groups of patients equally satisfied with the results.
The results show that a year later, both groups of patients had an equally low rate of symptoms and were equally satisfied with the overall situation of their knee. Both groups of patients said they believed their knee felt better than before the operation.
When asked if they would choose the same procedure again, 93% of the partial meniscectomy group said they would, as did 96% of the sham procedure group.
The researchers concluded:
In this trial involving patients without knee osteoarthritis, but with symptoms of a degenerative medial meniscus tear, the outcomes after arthroscopic partial meniscectomy were no better than those after a sham surgical procedure (essentially a ‘placebo’).
Speaking of the impact the study is likely to have, lead author Raine Sihvonen, a specialist in orthopedics and traumatology at Hatanpää Hospital in Tampere, southern Finland, says: ”It’s difficult to imagine that such a clear result, would result in no changes to treatment practices.”
He explains that in nearly all Western countries, this operation is now the most common surgical procedure after cataract surgery, adding that:
“By ceasing the procedures which have proven ineffective, we would avoid performing 10,000 useless surgeries every year in Finland alone. The corresponding figure for US is at least 500,000 surgeries.”
Co-author and state adjunct professor Teppo Järvinen, of the Helsinki University Central Hospital, says: ”Based on these results, we should question the current line of treatment according to which patients with knee pain attributed to a degenerative meniscus tear are treated with partial removal of the meniscus, as it seems clear that instead of surgery, the treatment of such patients should hinge on exercise and rehabilitation.”
Discovery of New Knee Ligament.
Earlier this year, an important discovery about knee anatomy made its mark when knee surgeons in Belgium for the first time described a new knee ligament called the anterolateral ligament (ALL). At University Hospitals Leuven, two surgeons have for the first time given a full anatomical description of the ALL. The new ligament is thought to play an important role in anterior cruciate ligament (ACL) tears.
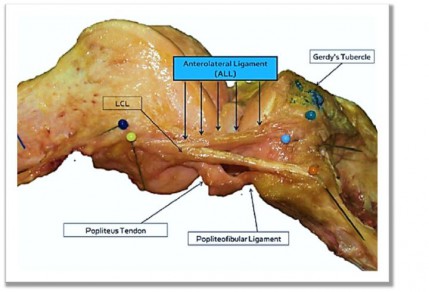
Figure 3. The “New” ALL Ligament.
It has been seen before, and labeled with many names. However, what makes it new is that is has been given a common name and its functions are now known.
Orthopedic surgeons Dr. Steven Claes and Prof. Johan Bellemans and colleagues, wrote about some of their findings in a recent issue of the Journal of Anatomy. For the last 4 years, the two surgeons have been researching ACL tears to find out why, despite undergoing successful ACL repair surgery and rehabilitation, some patients still experience ‘pivot shift,’ where the knee sometimes gives way. This can occur to athletes while playing. It can also affect weekend warriors.
‘Pearly band’ first described in 1879.
Their enquiries began with an 1879 article by the French surgeon Segond, who suggested that the front of the human knee had an additional “pearly, resistant, fibrous band.” Until now the mysterious “pearly band” has been given various confusing names, but “no clear anatomical description has yet been provided,” wrote the authors. So, using macroscopic dissection techniques, they carried out in-depth examinations of 41 cadaver knees and found the new ligament in all but one of them. They wrote:
“The ALL was found to be a distinct ligamentous structure at the anterolateral aspect of the human knee with consistent origin and insertion site features.”
Researchers propose that the ALL controls the rotation of the tibia, one of the two bones in the lower leg, and, given its structure and location in the knee, that pivot shift may be caused by an injury to the ALL.
They have since carried out some research that appears to confirm this.
The findings question current views about serious ACL injuries and could signify a breakthrough in the treatment of patients with such injuries. Doctors are already working on a technique to correct ALL injuries and hope it will be ready in a few years’ time.
ACL tears are common among athletes who practice pivot-heavy sports, such as basketball, skiing and football, or in sports where the participants are required to do repeated jump stops and cuts, such as soccer, tennis and volleyball.’ A recent study from the US and published in the Journal of Athletic Training, found that because they are more prone to landing in a knock-kneed position, women are more likely to tear the ACL than men.
Researchers say that women are nearly four times more likely to suffer from a tear to the ACL (anterior cruciate ligament) in the knee than men, but that it may be prevented by a different ‘landing strategy.’ The injury causes the knee to swell, and the joint becomes too painful to bear weight.
 Figure 4. This picture shows a Biomechanical model of a female using a “knock-kneed” technique, experiencing high frontal plane knee loading during a jump landing.
Figure 4. This picture shows a Biomechanical model of a female using a “knock-kneed” technique, experiencing high frontal plane knee loading during a jump landing.
It is known that people who hurt themselves tend to look stiff when they land and that the combined ‘knee loading’ from multiple directions is likely causing the injury, but it was not clear initially why women had more injuries than men.
Women are more ‘knock-kneed’ than men.
For this research, the study authors analyzed 82 physically healthy men and women using motion analysis software, to determine exactly how they landed when carrying out a series of jumping exercises. The researchers found that both men and women landed ‘stiffly,’ which can potentially lead to ACL injuries. However, women were 3.6 times more likely to land in a “knock kneed” position, which could be a critical factor causing gender disparity in ACL injuries.
They found that both men and women seem to be using their quad region the same, so that couldn’t explain why females are more at risk.
Using motion analysis, they were able to pinpoint that this inability to control the frontal-plane knee loading – basically stress on the knee from landing in a knock-kneed position — is a factor more common in women. Future research may isolate why women tend to land this way, but it could in part be because of basic anatomy. Women have wider hips, making it more likely that their knees come together after jumping.
Ongoing future research will focus on high school athletes in order to determine how ACL injuries can be prevented through warm-up techniques and improved landing strategies. The researchers are trying to create a prevention strategy that is sustainable and will be widely used by high school coaches.
Many athletes do come back from an ACL injury, but it is a long road. And, the real worry is that it leads to early onset osteoarthritis, which then impacts their ability to stay physically active. Osteoarthritis is the most common form of arthritis, affecting millions of people around the world.
While osteoarthritis can damage any joint in your body, the disorder most commonly affects joints in your hands, neck, lower back, knees and hips. Osteoarthritis gradually worsens with time, and no cure exists. But osteoarthritis treatments can slow the progression of the disease, relieve pain and improve joint function.
Rheumatoid arthritis is a chronic inflammatory disorder that typically affects the small joints in your hands and feet. Unlike osteoarthritis, rheumatoid arthritis affects the lining of your joints, causing a painful swelling that can eventually result in bone erosion and joint deformity.
An autoimmune disorder, rheumatoid arthritis occurs when your immune system mistakenly attacks your own body’s tissues. In addition to causing joint problems, rheumatoid arthritis sometimes can affect other organs of the body — such as the skin, eyes, lungs and blood vessels.
Although rheumatoid arthritis can occur at any age, it usually begins after age 40. The disorder is much more common in women than in men. Treatment focuses on controlling the symptoms and preventing joint damage.
Osteoarthritis (OA) and rheumatoid arthritis (RA) are distinguished by cartilage degeneration and bony overgrowth. OA affects approximately 13.9% of adults who are ≥25 years of age. The incidence of OA rises with age, with estimates that OA affects 12.4 million adults ≥65 years of age. OA occurs more frequently in women, particularly after reaching 50 years of age. Women are also at greater risk for developing OA in the knee or hip.
RA is an autoimmune condition characterized by inflammation, usually in bilateral joints, and systemic features, such as fatigue or fever. RA is estimated to affect 1.5 million adults. RA sufferers are typically younger than those who develop OA, with RA occurring between 20 to 30 years of age, and the incidence peaking at 35 to 50 years of age. The incidence of RA is higher in women with a higher lifetime risk (3.6%) compared to men (1.7%).
While there is no cure for OA or RA, treatments that slow or halt the progression of RA are available. Unfortunately, the same is not true for OA, where current pharmacologic treatment focuses on symptomatic relief.
Changes to bones (broken) and connective tissues (ligaments and tissues) often lead to osteoarthritic processes that may take years to become symptomatic. I broke both my ankles three-and-a-half years ago, and now have osteoarthritic symptoms (particularly a good deal of pain). They will worsen over time.
Young athletes can expect that this OA process may occur if they have such injuries to knees, ankles, shoulders, legs, and arms. It may take several years for the symptoms to occur, and perhaps, new treatments beyond the use of painkillers may be discovered for OA that will alleviate the symptoms more successfully. Such research is ongoing.
Related Articles:
Mike (Editor-in-Chief) is a 1970 graduate of the University of Oregon where he attended the Honors College and received all-conference honors as a swimmer. After college, Mike ran for the Oregon Track Club and narrowly missed qualifying for the US Olympic Trials in the marathon. He continues his involvement in sports with near-daily swimming or running workouts, occasional masters swim competition (where he has received two Top-10 World rankings), providing volunteer coaching to local triathletes and helping out with FishDuck.com.
Mike lives on 28 acres in the forest near Sandpoint, Idaho, where he has served as a certified public accountant for most of his working career. His current night job is writing novels about Abby Westminster, the only known illegitimate daughter of Britain’s finest secret agent who has to bring down arch-villains plotting dastardly deeds. And, yes, Abby is also a DUCK!