Sports medicine
All You Wanted to Know About Drugs and Doping in Sports – Part Two
Figure 1. Article by NeuroDocDuck
 Figure 2. Suspicions of doping persist in athletics. Those suspicions are too often true.
Figure 2. Suspicions of doping persist in athletics. Those suspicions are too often true.
With steroids easy to buy, testing weak and punishments inconsistent, college football players are packing on significant weight — 30 pounds or more in a single year, sometimes — without drawing much attention from their schools or the NCAA in a sport that earns tens of billions of dollars for teams.
Rules vary so widely that, on any given game day, a team with a strict no-steroid policy can face a team whose players have repeatedly tested positive.
An investigation by The Associated Press — based on interviews with players, testers, dealers and experts and an analysis of weight records for more than 61,000 players — revealed that while those running the multibillion-dollar sport say they believe the problem is under control, that control is hardly evident.
Football’s near-zero rate of positive steroids tests is not an accurate gauge among college athletes. Random tests provide weak deterrence and, by design, fail to catch every player using steroids. Colleges also are reluctant to spend money on expensive steroid testing when cheaperones for drugs like marijuana allow them to say they are doing everything they can to keep drugs out of football.
While other major sports are beset by revelations of steroid use, college football has operated with barely a whiff of scandal. Between 1996 and 2010 — the era of Barry Bonds, Mark McGwire, Marion Jones and Lance Armstrong — the failure rate for NCAA steroid tests fell even closer to zero from an already low rate of less than 1 percent.
The AP’s investigation, drawing upon more than a decade of official rosters from all 120 Football Bowl Subdivision teams, found thousands of players quickly putting on significant weight, even more than their fellow players did. The information compiled by the AP included players who appeared for multiple years on the same teams.
For decades, scientific studies have shown that anabolic steroid use leads to an increase in body weight. “Weight gain alone does not prove steroid use, but very rapid weight gain is one factor that would be deemed suspicious,” said Kathy Turpin, senior director of sport drug testing for the National Center for Drug Free Sport, which conducts tests for the NCAA and more than 300 schools.
Yet the NCAA has never studied weight gain or considered it concerning its steroid testing policies, said Mary Wilfert, the NCAA’s associate director of health and safety.
The NCAA attributes the decline in positive tests to its year-round drug-testing program, combined with anti-drug education and testing conducted by schools.
We already know from Part One of this series that a number of factors including genetics, and diet and training can cause quick weight gain. However, very fast growth can be suspicious, although not always supported by scientific evidence.
EXCEPTIONAL WEIGHT GAIN
The AP’s analysis found that, regardless of school, conference and won-loss record, many players gained weight at exceptional rates compared with their fellow athletes and while accounting for their heights.
Adding more than 20 or 25 pounds of lean muscle in a year is nearly impossible through diet and exercise alone, said Dan Benardot, director of the Laboratory for Elite Athlete Performance at Georgia State University.
In nearly all the rarest cases of weight gain in the AP study, players were offensive or defensive linemen, hulking giants who tower above 6-foot-3 and weigh 300 pounds or more. Four of those players interviewed by the AP said that they never used steroids and gained weight through dramatic increases in eating, up to six meals a day. Two said they were aware of other players using steroids.
“I ate 5-6 times a day,” said Clint Oldenburg, who played for Colorado State starting in 2002 and for five years in the NFL. Oldenburg’s weight increased over four years from 212 to 290.
Oldenburg told the AP he was surprised at the scope of steroid use in college football, even in Colorado State’s locker room.
“There were a lot of guys even on my team that were using.” He declined to identify any of them.
The AP found more than 4,700 players — or about 7 percent of all players — who gained more than 20 pounds overall in a single year. It was common for the athletes to gain 10, 15 and up to 20 pounds in their first year under a rigorous regimen of weightlifting and diet. Others gained 25, 35 and 40 pounds in a season. In roughly 100 cases, players packed on as much 80 pounds in a single year.
In at least 11 instances, players that AP identified as packing on significant weight in college went on to fail NFL drug tests. Nevertheless, professional football’s confidentiality rules make it impossible to know for a certainty which drugs were used and how many others failed tests that never became public.
Even though testers consider rapid weight gain suspicious, in practice it does not result in positive testing. Ben Lamaak, who arrived at Iowa State in 2006, said he weighed 225 pounds in high school. He graduated as a 320-pound offensive lineman and said he did it all naturally.
“I was just a young kid at that time, and I was still growing into my body,” he said. “It really was not that hard for me to gain the weight. I love to eat.”
In addition to random drug testing, Iowa State is one of many schools that have “reasonable suspicion” testing. That means players can be tested when their behavior or physical symptoms suggest drug use. Despite gaining 81 pounds in a year, Lamaak said he was never singled out for testing.
The associate athletics director for athletic training at Iowa State, Mark Coberley, said coaches and trainers use body composition, strength data and other factors to spot suspected cheaters. Lamaak, he said, was not suspicious because he gained a lot of “non-lean” (i.e., fat) weight.
However, looking solely at the most significant weight gainers also ignores players like Bryan Maneafaiga.
In the summer of 2004, Bryan Maneafaiga was an undersized 180-pound running back trying to make the University of Hawaii football team. Twice — once in pre-season and once in the fall — he failed school drug tests, showing up positive for marijuana use but not steroids.
He had started injecting stanozolol, a steroid, in the summer to help bulk up to a roster weight of 200 pounds. Once on the team, he would occasionally inject the milky liquid into his buttocks the day before games.
“Food and good training will only get you so far,” he told the AP recently.
Maneafaiga’s former coach, June Jones, said it was news to him that one of his players had used steroids. Jones believes the NCAA does a good job rooting out steroid use.
TESTING, DISCIPLINE ARE INCONSISTENT
In practice, though, the NCAA’s roughly 11,000 annual tests amount to a fraction of all athletes in Division I and II schools. Exactly how many tests are conducted each year on football players is unclear because the NCAA has not published its data for two years. Moreover, when it did, it periodically changed the formats, making it impossible to compare one year of football to the next.
Even when the NCAA tests players, experts like Catlin say it is easy enough to anticipate the test and develop a doping routine that results in a clean test by the time it occurs. NCAA rules say players can be notified up to two days in advance of a test, which Catlin says is plenty of time to beat a test if players have designed the right doping regimen. By comparison, Olympic athletes are given no notice.
Most schools that use Drug Free Sport testing service do not test for anabolic steroids, Turpin said. Some are worried about the cost. Others do not think they have a problem. In addition, others believe that since the NCAA tests for steroids their money is best spent testing for street drugs, she said.
Doping is a bigger deal at some schools than at others.
At Notre Dame and Alabama, the teams that competed for the national championship in January, players do not automatically miss games for testing positive for steroids. At Alabama, coaches have wide discretion. Notre Dame’s student-athlete handbook says a player who fails a test can return to the field once the steroids are out of his system.
The University of North Carolina kicks players off the team after a single positive test for steroids. Auburn’s student-athlete handbook calls for a half-season suspension for any athlete caught using performance-enhancing drugs.
At UCLA, home of the laboratory that for years set the standard for cutting-edge steroid testing, athletes can fail three drug tests before being suspended. At Bowling Green, testing is voluntary.
At the University of Maryland, students must get counseling after testing positive, but school officials cannot discipline first-time steroid users. This policy only harms the student-athletes!
Only about half the student athletes in a 2009 NCAA survey said they believed school testing deterred drug use. As an association of colleges and universities, the NCAA could not unilaterally force schools to institute uniform testing policies and sanctions, Wilfert said.
Oregon’s previous drug policy allowed for testing when there was reasonable suspicion. A recent decision by the general counsel gives temporary permission for random testing.
ESPN the magazine’s report last April about the use of marijuana was based on interviews with 19 current or former Oregon players and officials, and it accompanied a larger piece that looked at marijuana use among college football players nationwide. Of course, sadly there was nothing sought or expressed about steroid use.
Last July, Oregon’s athletic department proposed the changes to strengthen its drug policy. Under it, student-athletes would be subject to random tests year-round, even during the summer. A secure number system will identify athletes for testing. While Oregon’s athletic department proposed the changes to strengthen its substance-abuse policy, the school actually lessened the penalty for student-athletes with a third positive test (but not for steroid users – see below).
In 2010, Oregon’s substance-abuse policy, obtained through a public records request by ESPN, indicated the “continuing use of tested-for drugs on two occasions beyond the initial positive test, the student-athlete shall be expelled from the team and shall lose all athletic grant-in-aid support beginning with the next academic term.”
However, under the new current policy, a third positive test only results in missing 50 percent of games played in a season. If a player’s ineligibility is not complete by the end of postseason play, it carries over to the next season.
Student-athletes receive counseling and education after a first positive test. A second positive test results in a “behavior modification contract” between the student and the coach. A third positive test results in suspension for half of the games (i.e., 50%) played in a season for that sport. Dismissal and loss of scholarship does not occur now until a fourth positive test.
For performance-enhancing drugs such as steroids, Oregon athletes face suspension after the first positive test, and dismissal after the second, which mirrors the NCAA’s penalties for performance-enhancing drugs.
Steroids
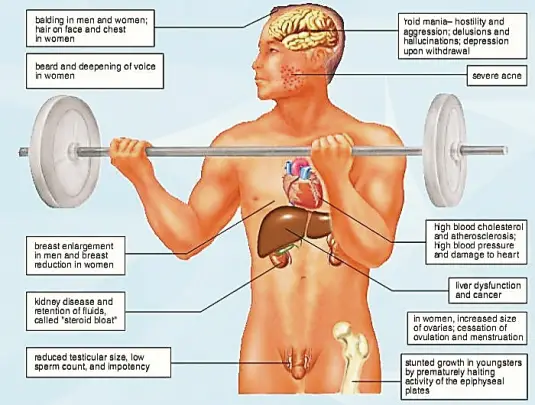
Steroids or anabolic steroids (anabolic-androgenic steroids -AAS) are synthetic derivatives of testosterone, a naturally occurring male anabolic hormone. The natural androgenic effects of testosterone include triggering of the maturity levels of the male reproductive system in the age of puberty. The triggering includes the growth of conditions such as voice deepening, growth of body hair, and development of body muscles. The anabolic effect of this hormone is to help in the retention of dietary protein that is useful for muscle development.
Prolonged use of high-dosage anabolic steroids to improve sports performance and athletic abilities can lead to serious side effects. Steroids can impact the testes and mammary glands in males. For females, steroid use affects the menstrual cycle and facial hair. Men and women who use steroids incur changes in blood cholesterol, changes in liver tissue and changes in the heart.
Males, who take steroids can experience infertility, lower sperm concentrations and reduced testicular size. These issues are reversible within several months of discontinued use. However, the use of steroids by a man can lead to the excessive development of his mammary glands, which is usually irreversible. The mammary glands may also begin to secret milk.
Females using anabolic steroids can experience an unusual amount of body and facial hair growth. Generally, irreversible changes include a reduction in the size of breasts, enlargement of the clitoris and the voice will deepen. The changes to a woman’s reproductive system may affect the development of mature ovum, ovulation and the menstrual cycle.
Both men and women on steroids can experience long-term damage to the liver. If one uses steroids, one is ingesting excess toxins that the liver must work to process. Steroid use causes the liver to develop blood-filled lesions, a condition known as peliosis hepatitis. In some extreme cases, the liver will fail and the person will die.
Anabolic steroids will reduce the level of HDL, commonly known as good cholesterol, in the body. HDL helps to remove cholesterol from the bloodstream. A constantly low level of HDL in the blood increases a person’s risk of developing coronary artery disease.
The structure of the heart can be changed, or damaged by steroids. Steroid use may also lead to increased plaque build-up, which can cause hardening of the arteries and high blood pressure. All of these conditions increase the risk of heart attack.
The American College of Sports Medicine (ACSM) reports that steroid use can lead to a change in mood and behavior, including increased aggression, hyperactivity and irritability. A person’s sexual drive can increase or decrease as well. ACSM advises that steroid use in young people can cause stunted growth. Steroid users may also notice extreme acne and a receding hairline.
Side effects from a longer course of systemic steroids
Figure 4. Adverse effects from a chronic course of systemic steroids.
|
SYSTEM |
ADVERSE EFFECTS |
| Skin | Increased risk of skin infections such as bacterial infections (e.g. cellulitis) and fungal infections (e.g. tinea (e.g., athlete’s foot and jock-itch), candida)Skin thinning resulting in easy bruising (purpura), skin tearing after minor injury and slow healing; these effects are most prominent on sun-exposed areas particularly the backs of the hands and the forearms. Stretch marks (striae), particularly under the arms and in the groin. Steroid acne: clusters of small spots on face, chest and upper back.
Excessive hair (hypertrichosis) and hair loss (alopecia)
Subcutaneous lipoatrophy (loss of fat under the skin surface) from injected steroid that does not go deep enough into the muscle.
|
| Weight | Redistribution of body fat results in moon face, buffalo hump and truncal obesity. Weight gain occurs in most patients on long-term steroids due to increased appetite and increased food intake. |
| Eyes | Glaucoma (increased intraocular pressure) can be due to corticosteroid eye drops as well as systemic steroids; often there is a family history of the disease. Posterior subcapsular cataracts in both eyes develop slowly; children are more susceptible than adults are. Swelling of eyelids and eye muscles resulting in bulging eyes (exophthalmos) is a rare side effect.Central serous chorioretinopathy describes swelling within the eye resulting in separation of the choroid from the retina.
|
| Vascular | Atherosclerosis (hardening of the arteries) in patients on long-term steroids may lead to:Ischemic heart disease: angina, heart attack (myocardial infarction), heart failure and atrial arrhythmiasStroke (cerebrovascular accident, CVA) and transient ischemic attack (TIA)Increased all-cause mortality. The effects of systemic steroids on atherosclerotic vascular disease may be due to complex metabolic changes, including:
Reduction in release of ACTH (adrenocorticotropic hormone) leading to elevated VLDL (very low density lipoprotein), LDL (low density lipoprotein) cholesterol and triglycerides, and lower HDL (high density lipoprotein) cholesterol
|
| Gastro-Intestinal | Peripheral insulin resistance and hyperinsulinemia. Corticosteroids may cause gastritis and peptic ulceration. Those also taking anti-inflammatory medications are at significantly increased risk of bleeding and should take acid-lowering medication to prevent this (e.g., a protein pump inhibitor such as omeprazole).
Systemic steroids may mask symptoms when athletes observe bleeding or when they become very ill from a perforation of the gut. It is then that patients sometimes first learn of gastrointestinal disease then.
|
| Liver | There is an increased risk of fatty liver (hepatic steatosis) on long-term steroids. |
| Circulatory | Sodium and fluid retention cause leg swelling and weight increase, usually in those with underlying heart or kidney disease. Increased blood pressure is common, especially with higher doses of steroid (more than 10mg of prednisone daily). Potassium loss may occur, causing general weakness. |
| Sexual Effects | Effects of continuous use of corticosteroids include: Irregular menstruation Lowered fertility in men and women
Possible increased risk of cleft palate in offspring of women taking steroids in pregnancy
|
| Orthopaedics | Osteoporosis (thinning of the bones) due to corticosteroids is common, particularly in smokers, postmenopausal women, the elderly, those who are underweight or immobile, and patients with diabetes or lung problems. Osteoporosis may result in fractures of the spine, ribs or hip joint with minimal trauma. These occur after the first year in 10-20% of patients treated with more than 7.5mg prednisone daily.Up to 50% of patients on long term, oral corticosteroids will develop bone fractures it is estimated. Osteonecrosis (destruction of bones such as the hip) is an uncommon but serious risk of high doses of steroids.
Muscle weakness (myopathy) often affects shoulders and thighs.
Vertebral fractures are more common in patients on steroids, even in those with normal bone density.
Discontinuing steroids prescribed to children reduce growth, which may not catch up after a prolonged course.
|
| NeuropsychiatricEffects | Psychological effects include mood changes, increased energy, excitement and euphoria. Psychiatric symptoms are less common but include hypomania, psychosis, delirium, memory loss and depression, which may require assessment and treatment. Insomnia and sleep disturbance is more likely with split doses and tends to be less severe if a single daily dose taken in the morning. |
| Neurological | Shakiness and tremor is more likely on higher doses. Headaches are common but serious raised intracranial pressure is rare. |
| Cortisol: Glucosteroids Treatment and Abuse | During and after steroid treatment, the adrenal gland produces less of its own cortisol, resulting from hypothalamic-pituitary-adrenal (HPA) axis suppression. Steroids may result in higher blood sugar (glucose) levels in patients with diabetes mellitus. Transient or persistent diabetes can affect previously nondiabetic patients, especially with higher daily doses of steroids. This needs treatment.
During and after steroid treatment, the adrenal gland produces less of its own cortisol, resulting from hypothalamic-pituitary-adrenal (HPA) axis suppression.
Steroids may result in higher blood sugar (glucose) levels in patients with diabetes mellitus.
Transient or persistent diabetes can affect previously nondiabetic patients, especially with higher daily doses of steroids. This needs treatment.
Glucocorticoids (cortisol – see below in article for discussion) result in inhibition of innate and acquired immunity and affect T cells, B cells, phagocytes and cytokines. This makes them effective in controlling a wide range of inflammatory diseases but also leads to adverse events. Increased susceptibility to internal infections, especially when high doses are prescribed (e.g., cancer tuberculosis).
Raised white cell count, especially due to an increase in circulating neutrophils
Reduced efficacy and increased risk of vaccines
Live vaccines such as polio or MMR (measles, mumps, rubella) should not be given to patients on higher doses of steroid (>20mg prednisone daily). It is safe and advisable to have other routine immunizations, such as an annual influenza vaccination.
Side effects from reducing the chronic dose include (or when using only when training and on gameday):
The lack of steroid response to stress such as infection or trauma could result in severe illness for up to twelve months after discontinuing steroids.
|
Nearly everyone on systemic steroids for more than a month suffers from, depending on daily dose, and how long they have been on systemic steroids, some adverse effects. Think about non-prescription levels of steroids in athletes who use such steroids. These effects may include any of the following problems, which are not listed in any particular order of importance.
For those taking prescribed systemic steroids, make sure she/he understands how to take the medicine safely. Regular monitoring during treatment may include:
- · Blood pressure
- · Body weight
- · Blood sugar
Discuss any side effects with one’s doctor.
Specific measures to reduce the chance of steroid-induced osteoporosis for patients that have taken, or expect to take, 7.5 mg or more of prednisone or prednisolone each day for a period of three months or longer – see below.
A DEXA bone scan measures bone density. Bone density gives an indication of the risk of fracture due to bone loss. Arrange to have a scan as one starts systemic steroids, and it should be repeated every year or as recommended by your physician.
Preventative treatment includes the following medications:
Adequate dietary intake (e.g. 3-4 dairy serves each day) or calcium tablets up to a daily intake of 1200mg calcium per day
- Vitamin D in various forms including monthly colecalciferol (D3) 50,000 units (1.25 mg)
- Estrogen (i.e. hormone replacement tablets in females that have had early menopause)
- Prescriptions often given for patients at higher risk of fracture include bisphosphonates like alendronate (Fosamax), etidronate, and zolidronic acid.
Treatment is most effective when started at the same time as the steroids, as most bone loss occurs within the first few months. This is most important for people taking more than 7.5mg of prednisone (or the equivalent dose of another oral corticosteroid) for three months or longer.
If the individual smokes, stop. Consume minimal alcohol. Take regular weight bearing exercise e.g. walking for 30 to 60 minutes each day.
Do not suddenly stop systemic steroids; the doctor will explain how gradually to come off them (particularly important if one has been on them for more than six weeks).
- No tapering is necessary if the course of steroids has been for less than one week.
- After taking a dose of 30 mg or more per day for 3-4 weeks, reduce the dose by 10 mg or less per day, taking days to weeks to stop altogether.
- A much slower reduction in dose may be required if the medication has been taken for several months or longer.
- Alternate day dosing may reduce side effects.
Steroids also affect the brain, and high doses can make people feel happy, euphoric, and ‘hyped-up’, with disturbance of sleep and even serious psychiatric illness such as mania, very aggressive behavior, and psychosis (delusions, paranoia, and loss of touch with reality). If steroid users are also taking other drugs that affect mood or brain function, these adverse effects can be far more common.
Steroids are extremely useful in the care of those with advanced cancer when short life expectancy from their condition means physicians are far more relaxed about long-term side effects.
Brain tumors often respond dramatically well to steroids. The reason is that the brain is contained in a bony box inside the skull and pressure can build up inside the head, resulting in headaches, sickness, drowsiness and other problems. Brain scans often show that a tumor the size of a walnut can be surrounded by a big immune reaction, with brain swelling and inflammation. Steroids reduce the additional swelling, often reversing symptoms and buying time – maybe a few weeks. The underlying cancer continues to grow and if the person finally begins to deteriorate and death often follows rapidly as the steroid dose is reduced.
So steroids are very powerful, with wide ranges of actions, producing dramatic effects ranging from pain relief to mood elevation, and if it were not for the very serious side effects they would be used even more often.
The body becomes dependent on steroids and when used in health care, most physicians reduce dosage gradually, even though they may start in an acute illness with a very high dose.
Here are a few facts about the immune system and cancer. For most of our lives, our immune system successfully fights cancerous cells, killing them as they develop. That is its job.
In fact, the only job Natural Killer cells have is to kill cancer cells and viruses. For cancer to develop, the immune system must either be worn out, or ineffective and unable to kill cancer cells as fast as they normally develop. Or if one must be exposed to a mass of cancer causing toxins, radiation or some such thing, that increase the rate of development of cancer cells to an abnormally high level that the immune system cannot handle.
One major cause of cause of cancer features a dysfunctional immune system. Either way, it is vital to strengthen the immune system in your battle against cancer. Especially if you are getting medical treatments that wipe out your immune system.
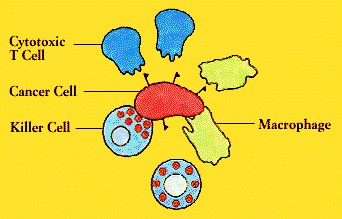
Immunity and Cancer The immune system provides one of the body’s main defenses against cancer. When normal cells turn into cancer cells, some of the antigens on their surface change. These new or altered antigens flag immune defenders, including cytotoxic T cells, natural killer cells, and macrophages.
Figure 5. T Cells, Killer Cells, and Macrophages attack a cancer cell.
According to one theory, patrolling cells of the immune system provide continuing bodywide surveillance, spying out and eliminating cells that undergo malignant transformation. Tumors develop when the surveillance system breaks down or is overwhelmed. Some tumors may elude the immune defenses by hiding or disguising their tumor antigens. Alternatively, tumors may survive by encouraging the production of suppressor T cells; these T cells act as the tumor’s allies, blocking cytotoxic T cells that would normally attack it.
Athletes can develop a lot of stress due to ecological (e.g., stress from coaches, learning the playbook and personal assignments within each play, outside pressures from home, girlfriends, wives, children, studies, family, other players and competitors, etc.) and to internal pressures (e.g., difficulty handling stress and anxiety, proneness to depression, personality disorders, substance abuse, and steroid abuse, etc.).
Natural steroids in the body come from cortisol metabolism, one of the substances released from the adrenal glands (the other is adrenaline for immediate use and lasting for two-to-five minutes before cortisol clicks in) during periods of stress.
Cortisol (made by adrenal glands) is a powerful anti-inflammatory hormone that, in small quantities, speeds tissue repair, but in larger quantities depresses your body’s immune defense system. Cortisol also reduces the rate at which lymphocytes [immune cells] multiply and accelerates their programmed cell death to protect further the body from this overreaction.
In fact, when cortisol is elevated during the alarm reaction there is almost a complete disappearance of lymphocytes from the blood. That is why your immune system is suppressed when we are under stress or taking corticosteroids. On the other hand, when circulating cortisol is low, its moderating effect on immune reactions is lost and lymphocytes circulate in excess. This creates more inflammation. Therefore, there is a range of normal cortisol secretion that exists in human beings. Staying within this range is elemental to proper immune system function. In addition, there is a relationship the immune system and behavior – they affect one another. Thus, too much and too little cortisol can cause behavioral problems.
Increased cortisol levels depress immune function, The part of the immune system most sensitive to the effects of cortisol are Natural Killer cells”. Immune system resistance plummets. Serious illnesses are often preceded by a major cause of stress.
There are many other reactions as well including adrenal gland “fatigue”. When adrenals become “fatigued” after being stressed, too little cortisol, and other, hormones are produced bringing on its own set of problems one major symptom being fatigue.
Essential fatty acids are the good fatty acids we need to get from food (e.g., fish) because we do not make them ourselves. Hormone-like cellular messengers called prostaglandins are derived from essential fatty acids. Cells respond to their environment through the action of prostaglandins.
Prostaglandins are short lived and very localized. Our diet is notably lacking in these good fats, especially since we decided sometime back that all fats were bad. Providing the raw materials, the fatty acids, in the first place is a nutritional issue. Most significant are the omega 3 fatty acids. Good prostaglandins inhibit “thick” blood, dilate blood vessels, are anti-inflammatory, control cell proliferation and enhance immune function. This positive action is inhibited by nutritional deficiencies, viruses, heavy metals, “bad” fats, and is further inhibited by red meat and sugar. ‘Bad’ prostaglandins do the opposite as in they promote “thick” blood, constricting blood vessels, are pro-inflammatory, promote cell proliferation and suppresses immune function. If someone is having a heart attack, they are making more ‘bad’ eicosanoids (that promote platelet aggregation and vasoconstriction) and not enough ‘good’ ones (that prevent platelet aggregation and promote vasodilation).
If an individual has high blood pressure (hypertension), they are producing more ‘bad’ eicosanoids (vasoconstrictors) and not enough ‘good’ ones (vasodilators). If one has arthritic pain, he/she is manufacturing more ‘bad’ eicosanoids (pro-inflammatory) and less ‘good’ ones (anti-inflammatory).
If there is cancer, the individual is creating more ‘bad’ eicosanoids (immune suppressing) and too few ‘good’ ones (immune stimulating). The EPA found that omega 3 marine lipid concentrate inhibits negative action and promotes the production of good prostaglandins. Stress negatively affects prostaglandin production. The stress hormone cortisol, produced by the adrenal glands when under stress, suppresses prostaglandin production. If one is overproducing corticosteroids, especially cortisol, it will bring all eicosanoid (prostaglandin) synthesis to a crashing halt – including the complete shutdown of the immune system.
Steroids act on the body much like cortisol. The benefits can be superb when steroids are used in treating illnesses. However, when there are too many steroids in the body, all kinds of things can go wrong in every organ system in the body – and can cause various diseases, including cancers.
Figure 6. Lyle Alzado believed that steroids cause his inoperable brain tumor. They did this by ruining his immune system. Other factors such as genetics, diet, stress dyscontrol, and personal things also probably played a role.
The cautionary tale about Lyle Alzado involves not only steroid abuse on a large and chronic basis, but also that none of us knows what is in our own DNA, and what kinds of things are floating around in our blood that can harm us when the immune system is suppressed. There is no sense in believing that anything bad will happen to somebody else; We are someone else’s somebody else!
There seems little point in needlessly playing Russian roulette with our health and our very lives!
Related Articles:
NeuroDocDuck (Dr. Driesen) is a doctor who specializes in neurology, and sports medicine. He is an Oregon alumnus, completing his medical education and training in the UK. He has been both a practicing clinician and professor, a well-known and respected diagnostician, an author, and has appeared on national television.
NeuroDocDuck is active in his profession, and stays current on all new trends in his field. He enjoys golf and loves his Ducks!