How would you feel to know that a significant part of your body was likely unknown to doctors who were treating an injury you suffered? Probably, surprise and then, perhaps, dismay! Further, how would you like to find out that after successful surgery and rehabilitation, your knee sometimes gives way? This can just as easily happen to the weekend superhero as well as to the trained athlete.
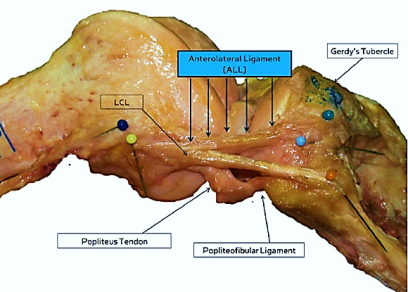
Earlier this year, an important discovery about knee anatomy made its mark when two knee surgeons at Belgian University Hospitals Leuven described, for the first time, a new ligament called the Anterolateral Ligament (ALL). They have given a full anatomical description of the new ligament that appears to play an important role in Anterior Cruciate Ligament (ACL) tears.
Google Images – http://www.npr.org/blogs/health/2013/11/07/243710560/surgeons-discover-quirky-knee-ligament-all-over-again
It was seen before and labeled with many names. However, what makes it new is that is has been given a common name, and its functions are now known.
Orthopedic surgeons Dr. Steven Claes and Prof. Johan Bellemans, et al., wrote about some of their findings. For the last four years, the two have been researching ACL tears to find out why, despite undergoing successful ACL repair surgery and rehabilitation, some patients still experience “pivot shift,” where the knee sometimes gives way. This can occur to virtually anyone and on any playing surface.
Their enquiries began with an 1879 article by the French surgeon Louis Segond, who suggested the front of the human knee had an additional ”pearly, resistant, fibrous band.” Until now the mysterious “pearly band” has been given various confusing names, but “no clear anatomical description has yet been provided,” write the authors.
Therefore, using macroscopic dissection techniques, they carried out in-depth examinations of 41 cadaver knees and found the new ligament in all but one of them (it is not unusual to find something missing, out of place, or sized differentially in the human body). They wrote, “The ALL was found to be a distinct ligamentous structure at the anterolateral aspect of the human knee with consistent origin and insertion site features.”
Researchers propose, given its structure and location in the knee, that the ALL controls the rotation of the tibia: one of the two bones in the lower leg, may be caused by an injury to the ALL.
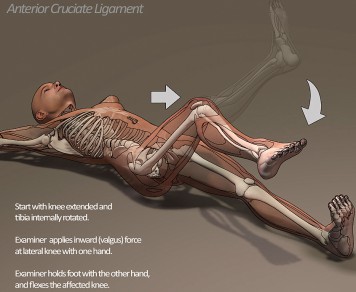
The Pivot Shift Test assesses ACL integrity and is performed with the patient supine (lying face up) and the knee in extension. One hand is placed on the lower leg, and the other hand is placed on the lateral aspect of the proximal tibia. The leg is rotated internally and a gentle ‘valgus force’ is applied while the knee is flexed. If the patient has an ACL tear, the tibia will visibly reduce on the femur with flexion of the knee.
There has been recent research that appears to confirm this. The findings question current views about serious ACL injuries and could signify a breakthrough in the treatment of patients. Doctors are already working on a technique to correct ALL injuries and hope it will be ready in a few years’ time.
ACL tears are common among athletes who are involved in pivot-heavy sports such as basketball, skiing and football. It is quite reasonable to think that some of these injuries may well include damage to the ALL.
A recent study published in the “Journal of Athletic Training,” found that because they are more prone to landing in a knock-kneed position, women are nearly four times more likely to tear the ACL — and consequently, ALLs — than men, but that it may be prevented by a different ‘landing strategy’.
ACL injuries are defined as “a tearing of the anterior cruciate ligament inside the knee joint.” The injury causes the knee to swell, and the joint becomes too painful to bear weight. These injuries are common in sports where the participants are required to perform repetitive maneuvers such as ’jump stops and cuts’. The list, therefore, expands to include soccer, tennis and volleyball.
It is known that people who hurt themselves, tend to look stiff when they land and that the combined ‘knee loading’ from multiple directions is likely causing the injury — but it is not clear why women had more injuries than men.
For this research, the study authors analyzed 82 physically healthy men and women using motion analysis software, to determine exactly how they landed when carrying out a series of jumping exercises.
The researchers found that both men and women landed ‘stiffly’ – which can lead to ACL injuries. Women, however, were 3.6 times more likely to land in a “knock-kneed” position — which could be a critical factor causing gender disparity in ACL injuries. They found that both men and women seem to be using their quad region the same, so that would not explain why females are more at risk.
Using motion analysis, the men in white were able to pinpoint that this inability to control the frontal-plane knee-loading stress on the knee from landing in that position — is a factor more common in women. Future research may find that it could be, in part, because of basic anatomy. Women have wider hips, making it more likely that their knees come together after jumping.
Of course, women are built differently than men. [Ed. note: PTL!]
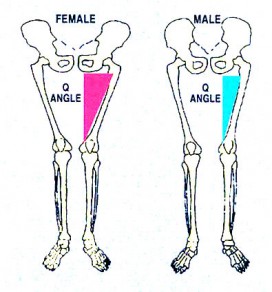
These differences are evident when examining the muscles and bones of their respective hips and legs. Compared with men, women have a wider pelvis. Their hips are more flexible and have more rotation. Their femur is tilted forward more at the top and is angled more toward the knee. Their lower leg is turned inward and angled more toward the knee.
Moreover, there are forces actually pushing outward. Women have less powerful thigh muscles, making the knee more dependent on the ligaments for stability. They have increased flexibility and hyperextension in their joints; and they have a narrower notch in the femur where their smaller anterior cruciate ligament is attached.
Why do these anatomic differences cause women to be more prone than men to ACL injuries? The small ACL often cannot handle the forces put on it during sports participation, so it tears. The ACL, then, serves as the main stabilizer of the knee.
Other contributing factors are associated with the sport and with the physical make-up of a woman. Her position, coordination, skill, talent, and coaching affect the way the female athlete uses her body and can affect whether she is at increased risk for ACL injury.
A poorly conditioned or overweight body puts more pressure on the knee joint and puts the athlete at greater risk for ACL injury. Hormonal levels at certain times during the menstrual cycle and extremely low percentage body fat cause the ACL to be more lax and, therefore, at increased risk for injury. Medical researchers are continuing to do investigations to find the exact reason for the disparity between the sexes and the best way to mitigate its effects.
In hopes of preventing ACL injury in females, some experts have suggested that basketball players, and other court sport participants, try to land on two feet rather than jump stopping and try to round off turns rather than cutting sharply.
The female athlete is very competitive and the mental drive to be the best burns brightly within her. For example, upon returning to competition after ACL reconstruction, a female University of Tennessee basketball player stated that she would do anything to win a national championship including tearing her ACL!
Competitive female athletes need to take measures to prevent ACLs. Finding ways to prevent those will ensure longer, more active, athletic participation for women.
Ongoing research focuses on how ACL injuries can be prevented using warm-up techniques and improved landing strategies. The researchers are trying to create a prevention strategy that is sustainable and will be widely used by coaches.
For athletes and nonathlete patients who would like to return to sports that require cutting, jumping, pivoting and/or contact, ACL reconstruction is recommended. Without reconstruction, the patient is at increased risk for recurrent “giving way” episodes (highly suggestive of ALL damage!!) and further damage to the articular surface and menisci, both of which may result in premature degenerative (e.g., osteoarthritic) changes.
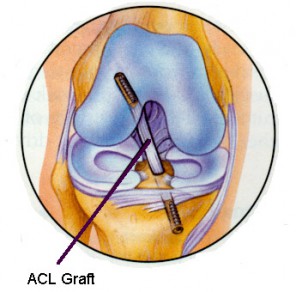
ACL reconstruction is one of the most common surgical procedures performed on the injured knee.
The anterior cruciate ligament is an intraarticular (within the joint) ligament, and as such heals poorly. For this reason, it is almost always reconstructed with a substitute ligament, rather than being repaired.
Transphyseal ACL reconstruction with hamstring tendon autograft has been shown to have 90%+ success rates in immature children and adolescents without disrupting the function of the distal femoral and proximal tibial physes.
The advantage of transphyseal reconstruction is the placement of the graft tissue in an isometric position, which provides better results, according to the literature. The potential disadvantage is angular or limb-length discrepancy caused by physeal violation. Controversy exists in allograft selection about whether bone or soft tissue passes into physes. The use of standard tunnels provides reliable results, but carries the risk of iatrogenic growth disturbance from physeal injury.
Another choice for ACL autograft is bone-patellar tendon-bone. Allografts (cadaver tissues) may also be used for ACL reconstructions. Allograft tendons take longer to remodel (up to two years) than autografts, and are associated with increased laxity and higher failure rates in this population.
Laxity of joints is also a risk factor for ACL tears. Patients with hyperextension at the knees are sometimes encouraged to wear a custom-fit knee brace after ACL reconstruction to help prevent reinjury.
Average return to sports time is nine to 12 months. Some studies have shown a negative impact on academic performance when ACL reconstruction is performed during the school year, but the potential risk of further damage to the knee must be considered when deciding to delay surgery. Many athletes of both sexes do come back from an ACL injury, but it is a long road. ALL damage complicates the prognosis.
Moreover, the real long-term worry is osteoarthritis (there will be a future article on osteoarthritis and rheumatoid arthritis in athletes and normal patients).
When athletes experience serious injuries, it’s equally important to pay attention to their mental health. If you have been injured and are feeling increased levels of stress or depression, you can connect with the mental health professionals at BetterHelp. All these components promote complete healing and I suggest you consider implementing the additional crucial mental aspects of treatment and recovery for your injuries.
Related Articles:
Chip Kelly Update: Everything's Good Again ...
Chip Kelly Update: Wailing and Gnashing of Teeth
Shock and Awe -- The Oregon Ducks' Football Hangover Effect
Despite Lopsided Score, Georgia State "Never Stopped Believing"
Hope Springs Eternal for Ducks
Incompetent Pac-12 Officials: How Do You Miss ALL of THIS?
NeuroDocDuck (Dr. Driesen) is a doctor who specializes in neurology, and sports medicine. He is an Oregon alumnus, completing his medical education and training in the UK. He has been both a practicing clinician and professor, a well-known and respected diagnostician, an author, and has appeared on national television.
NeuroDocDuck is active in his profession, and stays current on all new trends in his field. He enjoys golf and loves his Ducks!